A group of critical care, neurology, and education experts used the Delphi process to develop a list of 13 pediatric neurocritical care entrustable professional activities for pediatric critical care medicine.
Read the source article for this feature from Pediatric Critical Care Medicine.
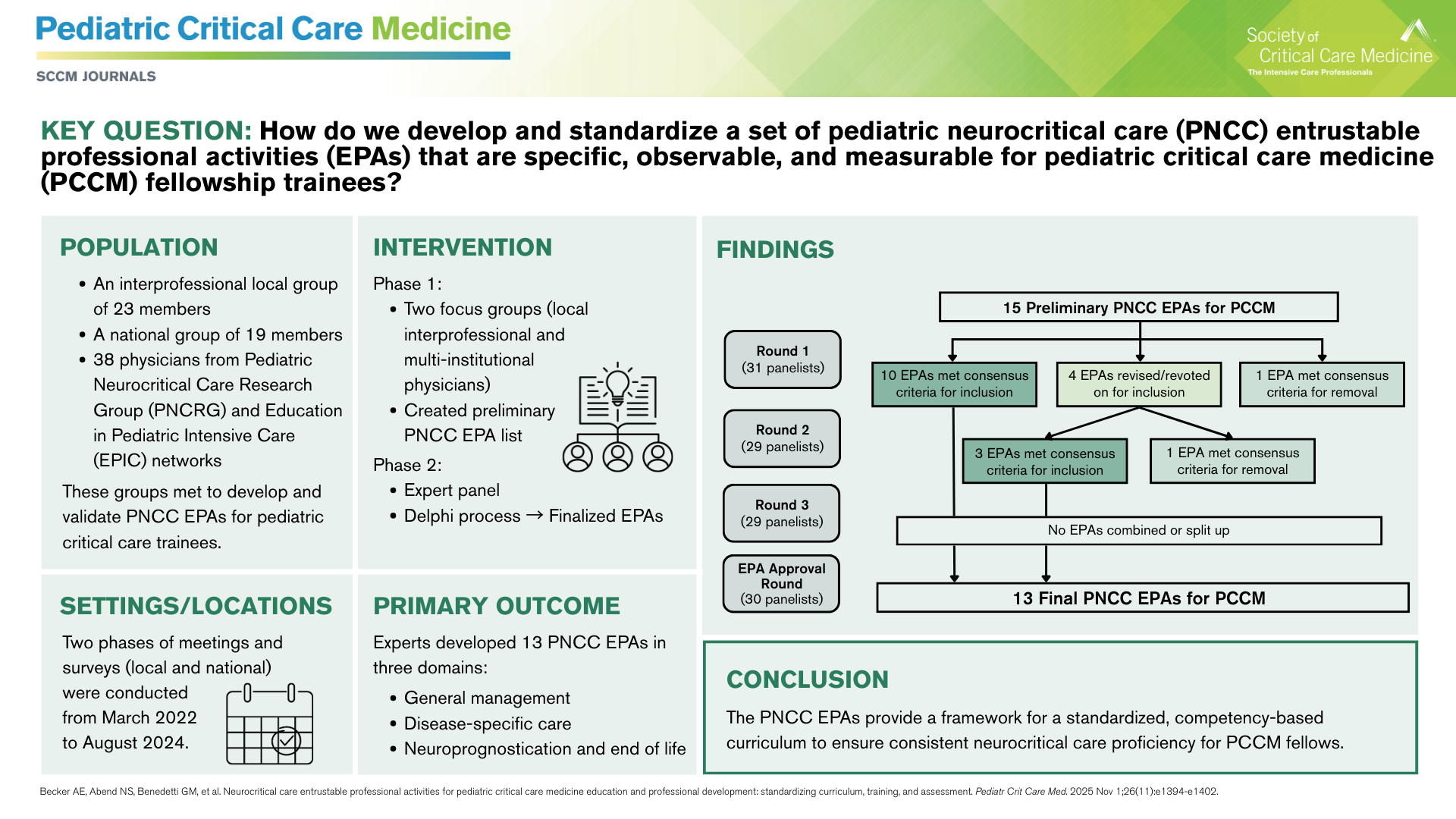
A group of critical care, neurology, and education experts used the Delphi process to develop a list of 13 pediatric neurocritical care entrustable professional activities (EPAs) for pediatric critical care medicine. The report and EPA list was published in the November 2025 issue of
Pediatric Critical Care Medicine.
1
“Entrustable professional activities are the everyday tasks that a person in their role should be able to do,” explained Andrew Becker, MD, a pediatric critical care medicine physician at K. Hovnanian Children’s Hospital at Jersey Shore University Medical Center. Dr. Becker was the project lead for this research during his pediatric critical care fellowship at the Children’s Hospital of Philadelphia, which he completed in June 2024.
He explained his interest in the project: “As a fellow, it’s hard to know how you’re doing, it’s hard to know how you’re being assessed, and it’s hard to get good feedback without specific things to ask about. I wanted a list of things that I could sit down with an attending the morning after a call or after a week of service and ask very specific questions.” The project also encompassed Dr. Becker’s research interest in competency-based medical education and clinical interest in pediatric neurocritical care.
The American Board of Pediatrics has outlined three EPAs for pediatric critical care medicine,
2 but they are quite broad, Dr. Becker said. “That makes it hard to develop curricula for training programs because what one program might value as important, another may not, and we want that to be consistent. It makes it hard to evaluate trainees as well, because feedback is best given, and assessment is best done, when you’re evaluating very specific things.”
Dr. Becker wanted to focus on a specific area—pediatric neurocritical care—and provide a more detailed list that would help both fellowship programs and trainees evaluate skills in which pediatric critical care medicine fellows need proficiency.
The Findings
Dr. Becker recruited both a local interprofessional focus group and a multi-institutional physician focus group to generate a list of EPAs. “The easiest thing to do would have been to get a group of PICU attending physicians where I was training to come up with a list,” Dr. Becker said. “But that’s not right because what is applicable and what is desirable at different training programs is not the same everywhere.”
Instead, he sought out a diverse group of experts from institutions of varying sizes and patient volumes and with and without neurology critical care teams. “I wanted people with pediatric neurocritical care expertise from PICU and neurology training. I wanted intensivists and pediatric neurologists. I wanted people like neurosurgeons who have a totally different training pathway. And lastly, I wanted people with an expertise in medical education.”
To finalize the list, a multi-institutional group of 38 physicians—36 pediatric critical care and/or neurology attending physicians and two pediatric critical care fellows—used the Delphi method. The Delphi facilitators did not set a goal for how many rounds they would need to reach a consensus or how many EPAs they should develop. “It’s really important that you don’t go in with any prespecified goals, and what happens, happens organically,” Dr. Becker said.
One aspect of the process that surprised him was that some people wanted more specificity for each EPA, while others wanted to keep each EPA broader. A consensus had to be reached not only on what EPAs to create but how to word each of them. The group agreed there needed to be wiggle room in the language to account for differences in training programs.
What’s Next
The final 13 EPAs were helpful to Dr. Becker personally as he completed his fellowship. “That was part of the goal of this whole project—this is now a list that a trainee and a training program can both look at and make sure they’re meeting these benchmarks. A group of very smart people with real expertise have agreed that these things are really important.”
While these EPAs are not required by an official body, they comprise a new educational tool for pediatric critical care medicine. Dr. Becker hopes that trainees will use them to gauge what they’re learning and that programs will use them to teach, evaluate, and provide feedback to fellows.
Future research teams could create EPAs in other specific areas of pediatric critical care medicine. “We started with neurology, with the hope that this is one of the first of many and that other groups would do similar things with other areas of interest within pediatric critical care.”
Table 2. Pediatric Neurocritical Care EPAs for Pediatric Critical Care Medicine Fellows
|
General management and principles
- Apply neuroanatomic and physiologic principles to perform and communicate key aspects of the patient’s neurologic examination
- Use neuroimaging and neuromonitoring technology and devices
- Recognize and apply sedation and procedural considerations specific to patients with neurologic disease
- Implement appropriate neuroprotective strategies to prevent secondary injury in patients with neurologic injury
- Recognize and manage neurologic and neuropsychiatric complications of critical illness and sequelae of neurologic injury
- Evaluate and co-manage patients with common perioperative neurosurgical and neurointerventional conditions
|
Disease-specific management
- Evaluate and manage patients with acute encephalopathy
- Manage patients with acute symptomatic cerebrovascular disease
- Manage patients with moderate and severe traumatic brain injury and increased intracranial pressure
- Manage patients with acute seizures, including status epilepticus
- Evaluate and manage patients with acute spinal cord and peripheral nervous system pathology, including neuromuscular weakness
|
Neuroprognostication and end-of-life care
- Demonstrate the communication skills necessary to discuss neuroprognostication with families
- Manage patients at the end of life
|