Fifteen-year-old Rowen Cartmill played basketball for Westside Christian High School’s freshman team on January 8, 2022. Three days later, he was in the pediatric intensive care unit (ICU) at Randall Children’s Hospital in Portland, Oregon, intubated, sedated, and paralyzed, and on extracorporeal membrane oxygenation (ECMO).
Fifteen-year-old Rowen Cartmill played basketball for Westside Christian High School’s freshman team on January 8, 2022. Three days later, he was in the pediatric intensive care unit (ICU) at Randall Children’s Hospital in Portland, Oregon, intubated, sedated, and paralyzed, and on extracorporeal membrane oxygenation (ECMO).
“He was so unstable that I was worried he was going to pass away that night,” said ICU Director Wendy Hasson, MD. “I couldn’t even talk to his family. I kept trying to talk to them about what I thought the night would hold, and he kept near-arresting. It was a constant state of emergency that night trying to keep him alive.”
Joshua A. Marks, MD, FACS, had a similar fear on the other side of the country when he first encountered 19-year-old Levi Oattes. Levi spent 384 days in the hospital—119 in the ICU. Rowen’s stay was 92 days, including 86 days on a ventilator, 62 in the ICU, and 56 on ECMO. The two patients survived thanks to the commitment and resilience of their care teams. Rowen, Levi, and the teams at Randall Children’s Hospital and Thomas Jefferson University Hospital are the 2023 recipients of the Society of Critical Care Medicine’s ICU Heroes Award.
Refusing to Give Up
 |
| Photo courtesy of Mauria Cartmill |
Rowen’s family members all tested positive for COVID-19 in December 2021. Their symptoms were fairly mild—cough and low fever. “Nothing too crazy,” said Mauria Cartmill, Rowen’s mother. After his basketball game in January, Rowen went home and immediately fell asleep, which was out of the ordinary. The next day he was fatigued, and the day after that, he had a 104° fever and tested positive for COVID-19. As his condition deteriorated, his parents sought help.
Because Rowen is six feet tall, his parents considered taking him to an adult hospital, but instead they chose Randall. Rowen had to stop multiple times to catch his breath during the walk from the car to the emergency department. He was immediately admitted to the ICU and started on oxygen, and hours later was intubated and started on ECMO.
Because severe COVID-19 is rare among children, the Randall team sought guidance from colleagues at Legacy Emanuel Medical Center, the adult hospital on their shared campus. They learned that prognoses for adults with similar conditions were poor, but a previously healthy child might expect a better prognosis.
.png) |
| Photo courtesy of Mauria Cartmill |
"I always say that my job as an ICU doctor is to anticipate the next step,” Dr. Hasson said. “We were at the point where there was no next step.” Rowen did stabilize for a couple of weeks, but his condition worsened again. His lungs, kidneys, and heart failed. The team was running out of ideas but did not give up on Rowen. They reached out to colleagues across the country and learned about a new double-lumen cannula for managing right heart failure, primarily in adult COVID-19 patients. The Randall team and Rowen’s parents thought it was the best option for Rowen.
They were right. Rowen’s condition began to improve soon after the cannula was inserted. He was decannulated from ECMO after nearly two months. Two weeks later, he was transferred to inpatient rehabilitation.
The Randall team’s collaboration and communication was key to Rowen’s survival, as was the care they practiced from the outset, according to Mauria Cartmill. “Their main priority was Rowen and how do we get him better,” she said. “They never gave us false hope, but they still kept trying, even when it seemed like there was nothing else that could be done. We’re so grateful for them and what they’ve done for our family. They are all heroes.”
 |
| Photo courtesy of Mauria Cartmill |
Dr. Hasson said that her colleagues and she did not only provide care, they received it from the Cartmills as well in the form of food, letters, and other signs of gratitude. “They could really see that this wasn’t just a job for us,” Dr. Hasson said. “It was really taking an emotional toll on us, taking care of Rowen and knowing that, despite our best efforts, we might lose him. While we supported them, they supported us too.”
Dr. Hasson and Mauria Cartmill remain in touch. On January 11, 2023, exactly one year after Rowen was first admitted to the ICU, Mauria texted Dr. Hasson a four-second video in which Rowen is once again playing basketball on his school team and making a basket.
“To have a case like Rowen’s really reminds you why you do what you do every day,” Dr. Hasson said. “We can take someone from the worst moment of their life and get them playing basketball again. That’s why we do what we do.”
 |
| Photo courtesy of Mauria Cartmill |
Compassion Amid the Chaos
 |
| Photo courtesy of Amy Oattes |
Amy Oattes does not dwell on the details of the accident that led her then 19-year-old son Levi to the brink of death. Levi was extricated from a motor vehicle crash and airlifted to Philadelphia’s Thomas Jefferson University Hospital with a left temporal bone fracture, multiple brain hemorrhages, bilateral rib fractures, pulmonary contusions, and burns covering 72% of his body. When she thinks about her son’s 384 days in the hospital, she thinks about his care team. “When we were in the SICU, what stood out to me the most was how invested everyone was in getting to know Levi,” Amy Oattes said. “Not medically, but they were asking me questions: What does he like to do? What are his interests? What are his hobbies? What channel does he want the TV on?”
The answer to that last question was ESPN, and the channel shouldn’t change unless there was a sports game on a different channel. Levi Oattes’ care team had copies of the schedules for Philadelphia’s major sports teams—the Eagles, the 76ers, and the Phillies—and they made sure to have the games on for him, even if he wasn’t paying attention. “In the beginning, we didn’t know if he was going to live a day or a week,” Amy Oattes said. “It could have been easy to look at the medical side of him, but they made a point to show compassion.”
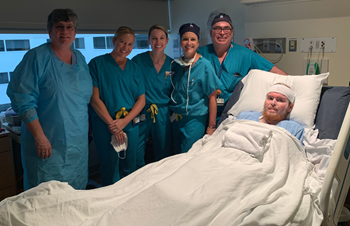 |
| Photo courtesy of Amy Oattes |
Dr. Marks, the hospital’s ICU director, was proud of that fact as well, in addition to the resilience the hospital’s team showed throughout Levi’s stay. “My initial reaction was, ‘I don’t know that he’s going to survive,’“ Dr. Marks said. “He was severely injured and, by any predictive model, even if you separate out his injuries, he probably shouldn’t have lived.” But he did. “Taking care of a critically ill patient for that many days, there’s burnout,” Dr. Marks said. “You can lose that light at the end of the tunnel. But the team didn’t give up, and some of that was driven by the patient, and his mom didn’t give up.”
 |
| Photo courtesy of Amy Oattes |
Amy Oattes said that never-give-up attitude was intentional. Each day she spent eight hours by her son’s side—reading him books, doing a play-by-play of a game on TV, or just making sure he knew she was there—and at the end of each day, her goal was to come home with something positive from the day. “Sometimes it was hard to come up with something positive,” she said, “but once you start looking for the positives, you kind of don’t look back.”
That is just what she and her son are doing. Levi, now 21, is back home with his family and focused on recuperating, by going to appointments with his care team and therapists and relaxing with his friends. When asked what winning the ICU Heroes Award meant to him, Levi joked that, for him, the recognition was for being the best at not dying.
As for Dr. Marks, the award was not only a huge honor, but also great inspiration. "It’s validation of the work that we’re doing as a team, day in and day out,” he said. “It really helps the team remember what it is that we’re doing and why we’re doing it. The fact that it’s coupled with the patient getting the award keeps us focused on why we’re here."


.png)




